Gynecomastia can hit teen boys at one of the most emotionally vulnerable times in their lives. Whether it shows up as puffy nipples or more developed breast tissue, it often leads to embarrassment, teasing, and withdrawal from sports or social activities. It may even lead to lasting emotional effects, such as social anxiety, depression, or avoidance behaviors that can linger well into adulthood. For many families in San Antonio, TX, this condition becomes more than a cosmetic concern-it becomes a question of confidence, identity, and quality of life.
Dr. Michael Baumholtz, a dual-board-certified Plastic Surgeon in San Antonio, regularly helps families navigate this decision. With expertise in both general and plastic surgery, he approaches every case with precision, compassion, and realistic guidance. He emphasizes open communication, patient safety, and individualized care that aligns with the family’s goals. If you're wondering whether to act now or wait, you're not alone-and you're in the right place to get clear, trustworthy information.
Understanding Teen Gynecomastia
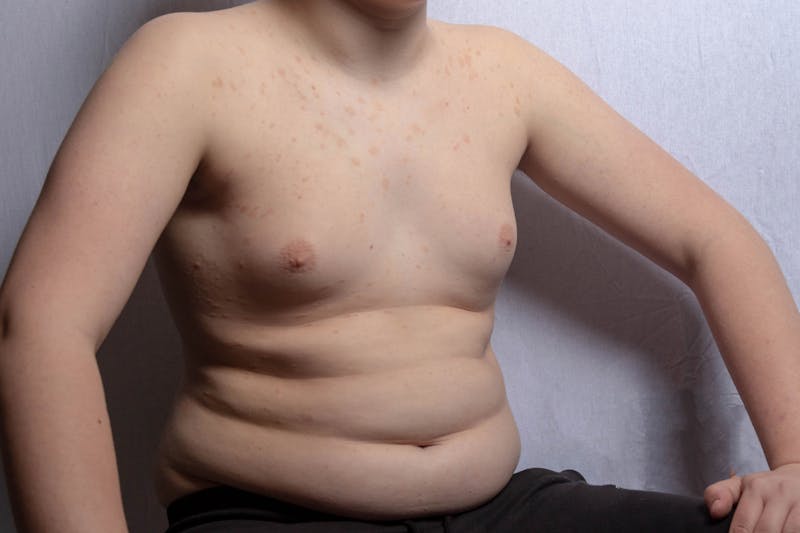
Teen gynecomastia is the enlargement of breast tissue in males, typically due to temporary hormonal changes during puberty. It's very common-affecting up to 70% of adolescent boys-but for most, it resolves naturally within a year or two. As hormones stabilize, the excess tissue may regress on its own without intervention. However, when the condition lingers beyond this window, it can have a deep impact on a teen’s emotional well-being, school experience, and willingness to participate in physical or social activities.
What’s important to know is that gynecomastia isn’t just about fat. It often includes firm, fibrous glandular tissue that doesn’t respond to weight loss or exercise. That tissue can be tender to the touch and may cause pain or discomfort. For teens dealing with persistent glandular gynecomastia, especially when it's noticeable or asymmetrical, the condition can feel devastating. Boys may attempt to hide their chest with oversized clothing, refuse to take their shirts off in public, or withdraw from team sports and other confidence-building experiences.
That’s why targeted treatment is often necessary-and why talking to a Plastic Surgeon like Dr. Michael Baumholtz is a smart first step. A consultation can clarify the type and severity of tissue involved and whether the condition is likely to resolve on its own or would benefit from surgical correction.
Why "Wait And See" Isn't Always Best
Telling a teen to “wait it out” can be painful when they’re already avoiding the pool, changing in gym class, or wearing hoodies in the summer. These coping behaviors are more than inconvenience-they can reflect deep emotional distress. The emotional toll becomes more serious than the physical one, especially when confidence takes a hit during formative years. Teens may experience teasing or bullying, which can affect academic performance, self-image, and peer relationships.
In Dr. Baumholtz’s experience, when gynecomastia has persisted for more than 12-24 months and begins to affect a teen’s social life or mental health, it’s time to consider intervention. Confidence isn’t something teens can put on hold until adulthood. He stresses that surgery is not about vanity- it’s about giving a young person the chance to feel comfortable in their own body.
"If a teen is missing out on life or feeling ashamed, it’s worth a conversation," says Dr. Baumholtz. "Sometimes the emotional weight is heavier than the physical one."
What Parents And Teens Should Know About Timing
Timing is everything. In many cases, it makes sense to observe for a year or two to see if gynecomastia will resolve naturally. Puberty is a process, and hormonal shifts can lead to temporary changes that may normalize with time. But what if it doesn’t?
If the glandular tissue remains firm and unchanged, or if the teen has stopped growing and their chest has a persistent breast-like shape, Dr. Michael Baumholtz may recommend surgery. He emphasizes the importance of puberty completion, but also recognizes that every case is personal. For instance, a 17-year-old who has completed physical development and has had stable symptoms for several years may be a better candidate than a 14-year-old still early in puberty.
In San Antonio, Dr. Baumholtz works closely with families to assess bone growth, maturity levels, and emotional readiness before recommending surgery. He takes time to answer questions, discuss expected outcomes, and ensure the teen is emotionally and psychologically prepared.
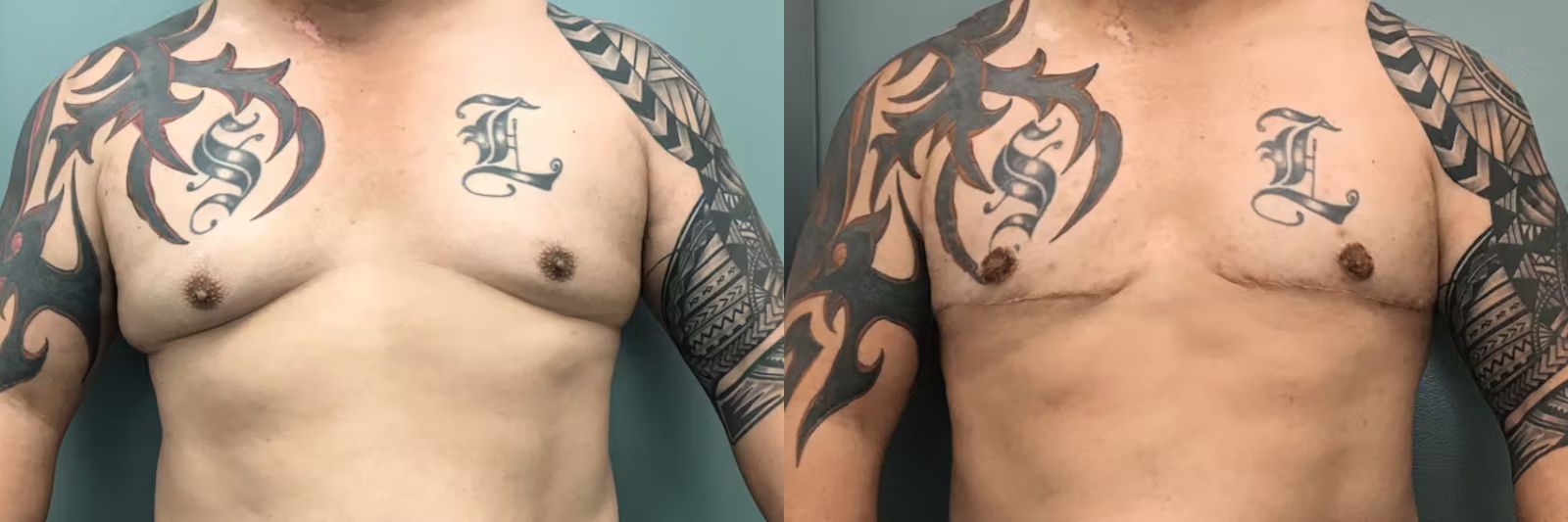
See Before and After Photos of Gynecomastia Surgery
How Dr. Michael Baumholtz Approaches Teen Gyno Cases
At his San Antonio plastic surgery practice, Dr. Baumholtz provides a comprehensive evaluation process. The consultation includes a detailed physical examination to determine the composition and distribution of the breast tissue. Some teens may have a more fatty appearance, while others have dense glandular tissue that cannot be reduced without surgery.
He also reviews the patient’s medical and medication history, as certain drugs or health conditions can contribute to gynecomastia. If needed, he may recommend lab tests or evaluations to rule out any hormonal imbalances or underlying endocrine disorders.
A key component of Dr. Baumholtz’s approach is speaking directly to the teen. He makes sure they understand what’s going on with their body and what options are available. This open dialogue helps teens feel empowered and engaged in their care. It’s not just about cosmetic change - it’s about helping a young person move forward with confidence.
When Surgery Makes Sense: Key Signs
Families might consider gynecomastia surgery if the condition has lasted more than 1–2 years with no signs of improvement. In some cases, the tissue may become firmer and more fibrotic over time, making it even less likely to resolve on its own. When a teen consistently avoids sports, pools, fitted clothing, or public changing areas, it may indicate deeper emotional discomfort.
Visible glandular mass or contour asymmetry - especially if it causes embarrassment or leads to teasing - can also signal that surgical intervention may be beneficial. Emotional stress, bullying, or anxiety that interferes with daily life, school participation, or social interaction should not be ignored.
When these signs are present, surgery is not cosmetic. It becomes a tool for emotional and social recovery, helping the teen re-engage with life without the burden of shame or self-consciousness.
The Surgical Process: What To Expect
Dr. Michael Baumholtz offers two proven surgical options, each tailored to the individual teen's anatomy and goals. Liposuction with arthroscopic gland removal is a minimally invasive technique ideal for mild to moderate cases. It uses small incisions placed discreetly along the chest creases to access and remove both fatty and glandular tissue. This approach avoids large scars and provides a more contoured, masculine appearance.
For severe cases involving significant excess skin or a more breast-like shape, Dr. Baumholtz may recommend a mastectomy with free nipple grafting. This procedure involves removing the excess tissue and repositioning the nipple for a natural appearance. It is less common in teens but appropriate for those with dramatic enlargement or weight-related skin excess.
All procedures are performed under general anesthesia in an accredited surgical facility. A board-certified anesthesiologist is always present, and Dr. Baumholtz ensures that each patient receives the highest standard of safety, comfort, and personalized care. He uses advanced instruments, gentle tissue handling, and thoughtful incision placement to reduce trauma and speed recovery.
Recovery, Results, And Real Relief
Recovery is often faster than families expect. Most teens are able to return to school in 3–5 days, with some resuming non-strenuous activity even sooner. Light activity can resume within two weeks, and full unrestricted activity, including sports and weightlifting, is typically allowed at six weeks.
Dr. Baumholtz prescribes a compression vest for six weeks post-op. This helps reduce swelling, supports the new chest contour, and enhances overall healing. His staff provides clear, step-by-step instructions on garment wear, wound care, medication use, and activity guidelines.
Follow-up visits are scheduled regularly to ensure optimal healing. If needed, scar care treatments are discussed, although most incisions fade significantly with time. The emotional impact of surgery is often immediate. Teens begin to stand taller, wear tighter clothes, and return to the activities they once avoided. For parents, seeing their child’s renewed confidence and emotional ease can be incredibly rewarding.
Common Misconceptions (And The Truth)
One common concern is whether it’s too early for surgery. Dr. Baumholtz reassures families that if the teen is physically stable and emotionally ready, early intervention can prevent years of emotional hardship. Another misconception is that the tissue might grow back. While recurrence is possible in rare cases, especially if hormonal issues persist, complete glandular removal makes this unlikely.
Scarring is another worry for many. With Dr. Baumholtz’s meticulous, minimal-incision technique, scars are often barely visible after healing. In many cases, they are hidden in natural creases and fade over time. If needed, scar treatments can further improve appearance.
These and other concerns are addressed fully during consultation, ensuring families feel confident, informed, and supported.
Why San Antonio Families Choose Dr. Baumholtz
Dr. Michael Baumholtz is known across Texas for his direct, respectful, and skilled care. Families choose him because he is dual board-certified in General and Plastic Surgery and brings fellowship training in hand and microsurgery. His combination of technical skill, safety-first mindset, and open communication has earned him a trusted reputation.
He offers personal, pre- and post-op access - not just a quick consultation. Every patient receives a customized care plan, hands-on follow-up, and the ability to reach Dr. Baumholtz directly if concerns arise. Many of his patients are referred by other providers or come to him after less satisfying experiences elsewhere. His ability to handle complex, revision, or sensitive cases is a standout feature of his San Antonio practice.
FAQs About Teen Gynecomastia Surgery
Can my son still grow out of gynecomastia even if he's almost done with puberty?
While late-puberty changes can occur, persistent gynecomastia beyond 1–2 years is unlikely to resolve without intervention. If your son’s symptoms have stabilized and are causing distress, it’s worth a surgical consult.
Will surgery affect chest muscle development later on?
No. Once healing is complete, teens can return to strength training and chest workouts. In fact, many feel more motivated to exercise post-surgery.
Is it safe to do this type of surgery before college or during summer break?
Yes, many families time surgery for school breaks. Summer is popular due to the six-week recovery period aligning with vacation schedules.
What if my teen is extremely anxious about the procedure itself?
Dr. Baumholtz takes extra time to talk through the process with both teen and parents. Anxiety is normal, and his team works to create a calm, reassuring experience from consult to recovery.
Does the procedure work equally well for overweight teens?
Yes, although surgical planning may differ. Dr. Baumholtz considers body composition, skin elasticity, and desired goals to ensure a tailored approach.
How do we know if the tissue is gland or just fat?
A clinical exam, and sometimes imaging, helps differentiate the two. Fat alone may improve with weight loss, but glandular tissue generally requires surgery.
What does recovery look like from a mental health standpoint?
Most teens experience significant emotional relief - less shame, more confidence, and better engagement with daily life. Dr. Baumholtz often hears from parents that it was a turning point for their child’s self-esteem.
Medical References
- Management of adolescent gynecomastia: an update - Acta Biomedica
https://pmc.ncbi.nlm.nih.gov/articles/PMC6166145/ - Pubertal gynecomastia incidence among 530,000 boys - Frontiers in Pediatrics
https://www.frontiersin.org/journals/pediatrics/articles/10.3389/fped.2024.1367550/full - Gynecomastia in Adolescent Males - PMC
https://pmc.ncbi.nlm.nih.gov/articles/PMC3706045/ - Gynecomastia in adolescent males: current understanding of its etiology, pathophysiology, diagnosis, and treatment - Annals of Pediatric Endocrinology & Metabolism
https://e-apem.org/journal/view.php?number=1034 - Clinical and Biochemical Phenotype of Adolescent Males with Gynecomastia - Journal of Clinical Research in Pediatric Endocrinology
https://jcrpe.org/articles/clinical-and-biochemical-phenotype-of-adolescent-males-with-gynecomastia/jcrpe.galenos.2019.2019.0027 - Use of Tamoxifen in Treatment of Pubertal Gynecomastia - Diabetes Metabolic Syndrome: Clinical Research & Reviews
https://journals.lww.com/dmms/fulltext/2024/19040/use_of_tamoxifen_in_treatment_of_pubertal.8.aspx - Treatment of adolescent gynecomastia - Journal of Pediatric Surgery
https://www.sciencedirect.com/science/article/abs/pii/S0022346809009798
Let's Talk About What's Right For Your Teen
Teen gynecomastia isn’t just a phase. For many, it’s an obstacle to living fully and confidently. At Baumholtz Plastic Surgery in San Antonio, TX, Dr. Michael Baumholtz offers real solutions, backed by experience and empathy. He understands that every teen’s journey is different, and he treats each case with the individual attention and respect it deserves.
Whether your son is ready for surgery or just beginning to ask questions, it starts with a conversation. Dr. Baumholtz will meet you where you are - and guide you through what’s next. A consultation is not a commitment to surgery - it’s a step toward understanding, reassurance, and clarity.
Your son’s confidence may depend on it.
To learn more or schedule an appointment, visit the website.
Further Reading
- Read Dr. Baumholtz Men Gynecomastia Procedure
- Read more about Male Chest Surgery Without Scars The Truth About Minimal Incision Gynecomastia Surgery
- Read more about How To Get Rid Of Puffy Nipples In Men: Surgical And Non-Surgical Options