Recovery after breast implant exchange - sometimes called breast implant remove and replace (BIRR) - is not one predictable experience. It is a process shaped by what was done surgically, how long the implants have been in place, how tissues have changed over time, and what each patient needs in order to heal well.
Many women pursue an exchange or revision years after their original breast augmentation. Anatomy, skin quality, scar behavior, and priorities are often very different than they were the first time.
Dr. Michael Baumholtz, plastic surgeon in San Antonio, Texas, approaches this reality in a steady, practical way. Recovery should be organized, individualized, and honest about tradeoffs. The goal is a plan a patient can follow without confusion - one that protects the operation and fits real life.
The operating room is only one part of the project. What happens afterward - walking, rest, incision care, support garments, and activity choices - plays a major role in how well the result holds up over time.
What “Breast Implant Exchange” Actually Includes
Patients often hear “exchange” and assume it means “swap the implant and go home.”
Sometimes that is close to the truth. Often it is not.
An implant exchange can include one or more of the following:
- Simple implant removal and replacement in the same pocket
- Capsule release (cutting tight scar tissue)
- Partial or total capsulectomy (removing scar tissue)
- Pocket modification to correct malposition
- Changing implant position (over the muscle to dual-plane/submuscular, or vice versa)
- Adding internal support (absorbable mesh) to stabilize the fold or repair
- Adding a breast lift (mastopexy) to restore nipple position and shape
Those details matter because what was done dictates what you feel and how long you need to protect the repair.
Video: Breast Implant Replacement
Why Recovery After Implant Exchange Can Be More Involved Than the First Augmentation
Many patients assume an exchange is easier than their first augmentation. Sometimes it is. Often it is not.
By the time a second or third surgery is needed, tissues may be:
- Thinner
- More stretched
- Less elastic
- More scarred
- More prone to implant movement
Gravity, weight changes, pregnancy, breastfeeding, exercise patterns, and aging leave their mark. None of this prevents a good outcome. It does mean repair work is common - and recovery must match the work performed.
Implant Malposition and Why It Changes Recovery
Implant malposition is common over time. It may include:
- Bottoming out (implant drops low)
- Lateral drift (implant moves toward the armpit)
- Symmastia (implants drift toward the midline)
- Double-bubble (fold mismatch creating a contour line)
- Visible asymmetry that wasn’t present early on
Correcting malposition often involves internal pocket work, which must heal undisturbed. That makes “protection” more important than it was in a straightforward first augmentation.
Dr. Baumholtz’s Recovery Framework
Recovery is organized around three pillars. The pillars stay consistent. The details are customized.
1) Comfort
Pain, nausea, and poor sleep derail recovery quickly.
A practical, multimodal approach is preferred:
- Non-narcotic medications as the foundation
- Short-term stronger medication only when needed
- Proactive nausea prevention
- Sleep support strategies
- Muscle discomfort addressed early when implants are under or partially under the muscle
The goal is not to “tough it out.” The goal is to stay functional enough to walk, hydrate, eat, and rest.
2) Movement
Movement begins early, but stays measured.
- Short, frequent walks start the day of surgery
- Walking continues at home
- Activity builds gradually based on energy and soreness, not forced milestones
Movement supports circulation and reduces clot risk.
3) Protection
Protection is non-negotiable.
Support bras, lifting limits, and incision care protect:
- The implant pocket
- The fold
- Internal sutures
- Any mesh support
- Any lift incisions
Impact exercise, bouncing, and massage are delayed when internal repairs need time to mature.
What Was Done Dictates What You Feel
Understanding the “why” behind sensations reduces anxiety.
If the exchange was straightforward in the same pocket:
Common sensations include:
- Pressure and tightness
- Swelling that shifts
- Mild soreness that improves relatively quickly
If capsule work was performed:
Expect more swelling and soreness because scar tissue was manipulated.
If implant position changed to dual-plane or submuscular:
Expect muscle-related tightness in the first week, which usually settles as the muscle relaxes.
If a breast lift was added:
Expect:
- More incision care
- More scar management
- A longer protective phase
If absorbable mesh or internal support was used:
Expect:
- Longer restrictions on impact and massage
- More emphasis on bra support and activity limits
This is why there is no universal recovery timeline.
Recovery Timeline: What Most Patients Can Expect
This is a realistic framework, not a guarantee. Dr. Baumholtz clears activity based on the exact surgery performed and how tissues are behaving.
✓ The First 48 Hours: Simple, Quiet, Supported
The goal is to keep recovery calm.
Most patients go home in a soft, front-closing support bra.
Priorities:
- Hydration
- Light meals
- Short walks every 1–2 hours while awake
- Back sleeping with the torso elevated
- Medications taken on schedule (do not chase pain)
Many patients describe pressure and fullness rather than sharp pain.
Home help matters. Childcare, pets, errands, and lifting should be delegated if possible.
✓ Days 3–7: Establishing a Rhythm
Tightness and soreness often peak early and then begin to settle.
Energy returns in waves.
Common expectations:
- A “good morning, tired afternoon” pattern
- Mild swelling shifts day-to-day
- Ongoing bra support full-time except for hygiene
Driving is usually reasonable once:
- No narcotics are being used
- Arm movement feels safe
- Reaction time is normal
Desk work may be possible within a week for simple exchanges. More complex repairs often deserve more rest.
The first follow-up focuses on:
- Incision status
- Early positioning
- Comfort
- Clear guardrails
Impatience is common here. Consistency matters more than intensity.
✓ Week 2: Gentle Forward Progress
By week two:
- Soreness continues to fade
- Sleep improves
- Daily activity feels less fragile
Scar planning begins, but scar “treatment” is not rushed. Early scar care is about protecting healing skin, not forcing a quick cosmetic change.
Massage may be allowed for a straightforward exchange once incisions are sealed and calm. If a lift, fold repair, or mesh support was used, massage is usually delayed.
Low-impact cardio may be allowed when cleared:
- Slow treadmill walking
- Stationary bike with low resistance
Side sleeping may return when comfortable and approved.
✓ Weeks 3-6: Structure Builds Confidence
This phase rewards discipline.
- Low-impact cardio gradually increases
- Normal arm use expands for daily tasks
- Lifting limits often remain in place
- Direct chest workouts still wait
Scar care becomes more active once incisions are closed and calm. A simple scar plan is usually the most effective because it is sustainable:
- Silicone-based scar therapy
- Gentle massage when approved
- Daily sun protection
South Texas heat matters. Moisture and friction can irritate incisions. Breathable fabrics and clean bra support make recovery easier.
✓ Six Weeks and Beyond: Back to Full Life With Guardrails
Around six weeks, many patients with a straightforward exchange can return to full activity with clearance.
Patients with:
- lift incisions
- significant capsule work
- mesh support
- major pocket tightening
may need more time.
Strength training typically resumes in phases:
- Lower body first
- Core after clearance (if no lift-related restrictions)
- Upper body gradually, avoiding direct chest strain until soft tissues are ready
Underwire bras may return once comfortable and cleared.
The goal is a normal life that does not feel fragile.
Scars: A Long Process, Not a Quick Judgment
Scars change over months.
Early phase priorities:
- Clean healing
- Avoiding tension and moisture
Once incisions are sealed and calm:
- Silicone scar therapy
- Gentle massage when allowed
- Sun protection every day
In San Antonio, sun protection is not optional. New scars darken easily and can stay darker if UV exposure is repeated.
Expect scars to mature over 12–18 months.
Breast Revision Before and After Photos
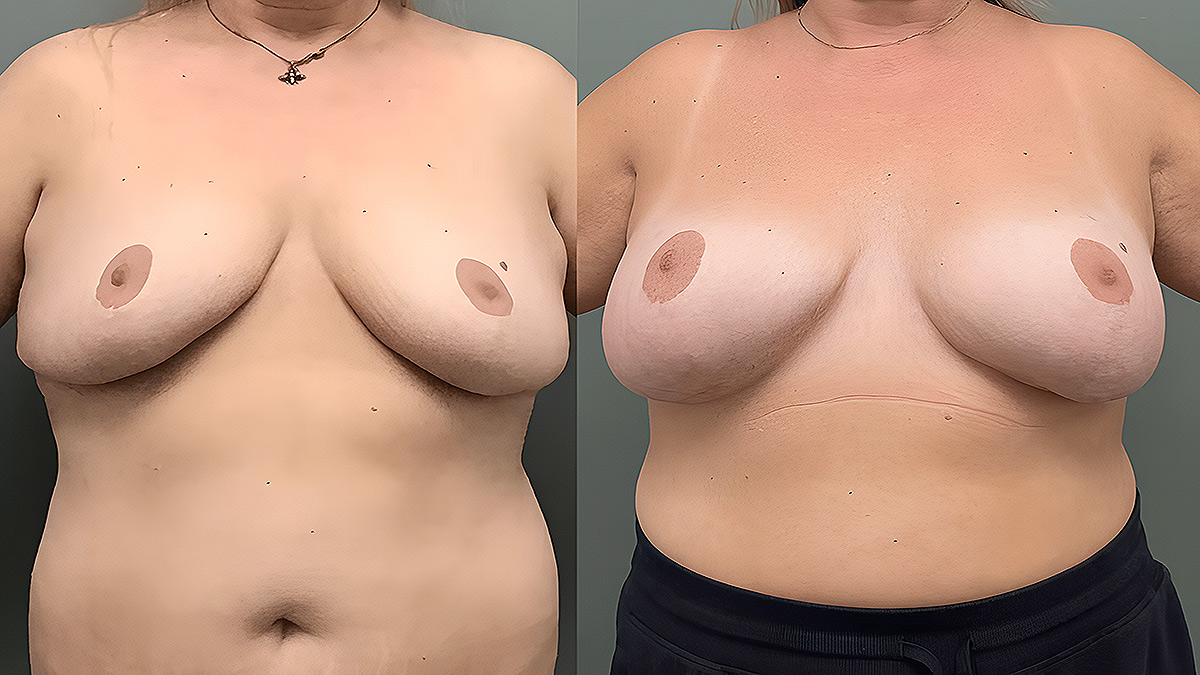
Visit Breast Revision Gallery for More Before and After Photos
Emotional Recovery Is Part of Recovery
Recovery is physical and emotional.
It is common to feel:
- relief
- pride
- worry
- impatience
Swelling hides shape. Asymmetries look worse before they soften. Progress is best measured week-to-week, not day-to-day.
Simple standardized photos (same lighting, same angle) can help patients see progress the mirror can hide.
Asking for help is not indulgent. It protects the repair.
Technique Choices That Affect Recovery
Technique influences how recovery feels and how results age.
Dr. Baumholtz commonly prefers:
- Inframammary fold incision for clean access in exchange cases
- Smooth implant options (avoids macro-textured devices)
- Meticulous sterile technique
- Funnel-assisted insertion when appropriate
- Selective absorbable mesh support when tissues are thin or repair stability needs reinforcement
These choices do not remove risk. They aim to reduce avoidable risk and increase long-term stability.
Work, Exercise, and Travel Planning
Recovery planning should reflect real life.
Work
- Desk work may return within a week for straightforward exchanges
- More complex cases often require longer downtime
- Jobs involving lifting, overhead movement, or heat exposure usually need a longer ramp
Exercise
- Walking immediately
- Low-impact cardio after clearance
- Strength training in phases
- Running and high-impact later, because bounce stresses healing tissues
Travel
Long car rides require:
- Bra support
- Hydration
- Walking breaks
- Avoiding heavy luggage
Red Flags to Know (Without Panic)
Patients should know what deserves a call.
Contact the office promptly for:
- Sudden increase in breast size on one side
- Rapidly increasing pain
- Spreading redness
- Fever over 101°F
- Foul drainage
- Shortness of breath
- Calf pain or swelling
Early communication prevents small issues from becoming bigger ones.
Follow-Up Is Part of the Procedure
Follow-up is not an add-on. It is part of the operation.
Early visits assess:
- incision healing
- early position
- swelling shifts
- comfort and medication plan
Later visits guide:
- activity progression
- scar care
- bra transitions
- long-term stability
Patients are encouraged to return with questions rather than carry uncertainty.
When a Touch-Up Makes Sense
Minor refinement can be part of long-term implant care.
Timing is deliberate. Tissues need time to settle before a small adjustment can be assessed accurately.
Early patience avoids chasing problems that resolve as swelling fades. If refinement truly adds value later, it is discussed clearly and approached safely.
Frequently Asked Questions
How long is recovery after breast implant exchange?
Many patients feel steady within 1–2 weeks after a straightforward exchange. Revisions involving lift incisions, pocket tightening, mesh support, or extensive capsule work often require a longer protective phase before unrestricted activity.
Is recovery easier than the first augmentation?
Sometimes. Often it is more involved because tissues are thinner, scar tissue is present, and pocket repairs need protection.
How painful is implant exchange recovery?
Most patients describe pressure, tightness, and soreness more than sharp pain. A multimodal pain plan and consistent bra support make the first week more manageable.
When can I drive?
When you are off narcotic medication, can move safely without guarding the chest, and can brake and steer comfortably.
When can I go back to work?
Desk work may be possible within a week for simple exchanges. If internal support, lift, or extensive capsule work was performed, more downtime is often wiser.
When can I start exercise?
Walking immediately. Low-impact cardio after clearance. Strength training resumes gradually and in phases. High-impact usually waits longer, especially after pocket repairs.
When can I start breast massage?
Timing depends on what was repaired. Straightforward exchanges may allow earlier massage once incisions are sealed. Lift, fold repair, or mesh support often delay massage to protect internal healing.
What kind of bra should I wear?
A soft, supportive, front-closing surgical or athletic-style bra is commonly used early. Underwire returns only after clearance and comfort.
When can I sleep on my side?
Back sleeping with elevation is preferred early. Side sleeping returns when comfortable and cleared, which varies by procedure and swelling.
How long do scars take to fade?
Scars mature over 12–18 months. Silicone therapy, massage when approved, and daily sun protection improve scar quality.
What are warning signs I should not ignore?
Sudden one-sided swelling, rapidly increasing pain, spreading redness, fever over 101°F, foul drainage, shortness of breath, or calf pain.
What if my implants feel high or tight at first?
That is common early on. Position and softness change as swelling fades and tissues relax. Follow-up visits help distinguish normal settling from issues that need action.
Medical References
- Swanson E. Prospective comparative clinical evaluation of outcomes and complications in breast augmentation and reoperation. Plast Reconstr Surg. 2013. - https://pubmed.ncbi.nlm.nih.gov/23806952/
- Maxwell GP, Gabriel A. Breast implant revision surgery: Concepts and options. Aesthetic Surg J. 2014. - https://academic.oup.com/asj/article/34/7/1033/201244
- Adams WP Jr. Capsular contracture: Etiology, prevention, and management. Clin Plast Surg. 2009. - https://pubmed.ncbi.nlm.nih.gov/19055967/
- Spear SL, Baker JL Jr. Classification of capsular contracture after prosthetic breast reconstruction. Plast Reconstr Surg. 1995. - https://pubmed.ncbi.nlm.nih.gov/7568488/
- Handel N, Cordray T, Gutierrez J, Jensen JA. A long-term study of outcomes, complications, and patient satisfaction with breast implants. Plast Reconstr Surg. 2006. - https://pubmed.ncbi.nlm.nih.gov/16936644/
- Pittet B, Montandon D, Pittet D. Infection in breast implants. Lancet Infect Dis. 2005. - https://pubmed.ncbi.nlm.nih.gov/15680779/
- Pannucci CJ, et al. Evaluation and management of venous thromboembolism risk in plastic surgery patients. Plast Reconstr Surg. 2011. - https://pubmed.ncbi.nlm.nih.gov/21196841/
- Bengtson BP, et al. Management of implant malposition and pocket revision principles. Aesthetic Surg J. 2011. - https://academic.oup.com/asj/article/31/6/649/194750
- Tebbetts JB. Dual-plane breast augmentation: Optimizing implant–soft-tissue relationships. Plast Reconstr Surg. 2006. - https://pubmed.ncbi.nlm.nih.gov/17099485/
- Jewell ML, et al. Use of acellular dermal matrix or absorbable mesh in breast surgery: Indications and outcomes. Aesthetic Surg J. 2017. - https://academic.oup.com/asj/article/31/7_Supplement/75S/258596
Closing
Breast implant exchange is common. Implant malposition over time is also common. Secondary and tertiary procedures are part of long-term implant care for many patients.
The key is aligning recovery with what was actually done and with the person healing from it.
The goal of BIRR is straightforward:
Heal safely, protect the repair, and return to regular life at a pace that supports long-term success.
That pace is dictated by biology and surgical details - not by a calendar alone.
If you are considering breast implant exchange or revision in San Antonio, schedule a consultation with Dr. Michael Baumholtz. Expect a clear plan, honest tradeoffs, and recovery guidance matched to your surgery.
All procedures carry risks. Individual results vary. Decisions are made case by case after examination and discussion of goals.
Further Reading
- Read more about Breast Implant Revision Procedure in San Antonio
- Read more about Capsular Contracture
- Read Dr Baumholtz's Blog on Types of Breast Implants
- Read Dr Baumholtz's Blog on What Is the Best Breast Implant?co
- Read Dr Baumholtz's Blog on Do Breast Implants Need To Be Replaced Every 10 Years?
- Read Dr Baumholtz's Blog on Fat Grafting or Implants: Which Is Best for You?