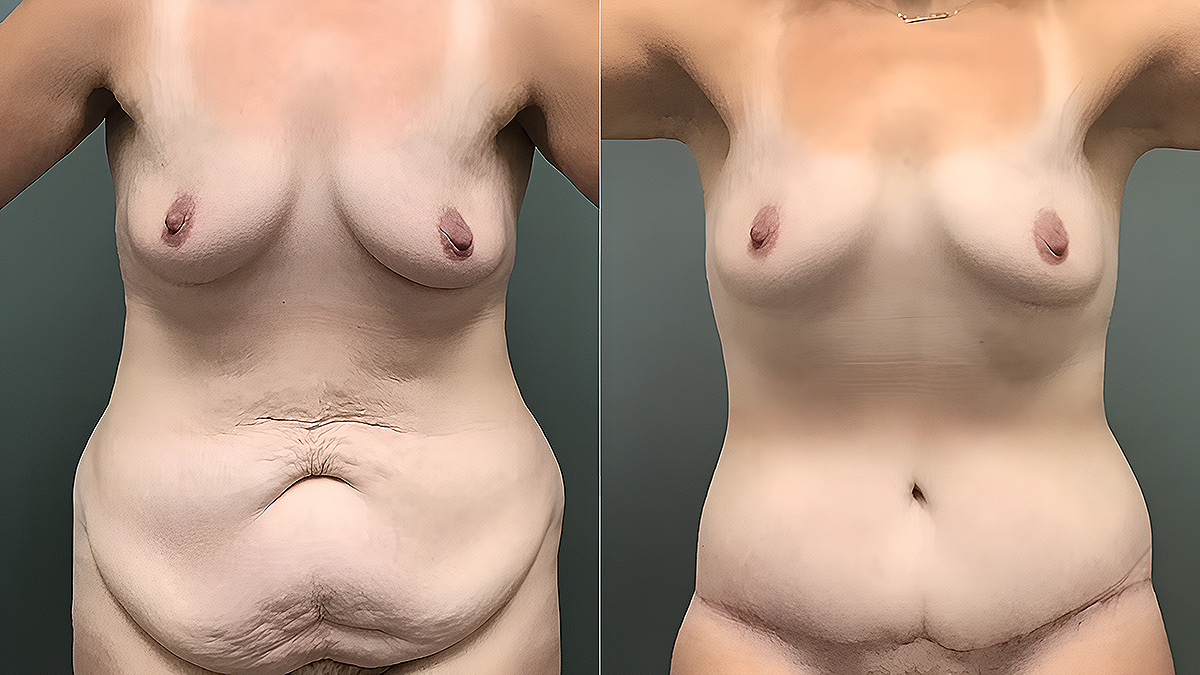
A clear guide to sleeping positions after a tummy tuck in San Antonio, Texas
Why Sleep Matters After Abdominoplasty
Most people preparing for a tummy tuck focus on the operation itself. What surprises many patients is how important sleep becomes during recovery.
The way a patient sleeps after abdominoplasty affects:
- tension on the muscle repair
- pressure on the incision
- swelling patterns
- comfort through the night
- how the abdomen feels the next morning
Sleep is when the body does much of its healing work. During sleep the body shifts hormones, reduces inflammation, and rebuilds injured tissue.
After abdominoplasty, sleeping position matters because the abdominal wall has been tightened. Lying flat too early pulls the abdomen into a stretched position.
That stretch can:
- increase tension on the muscle repair
- pull on the incision
- make breathing feel tight
- wake patients repeatedly during the night
Patients often notice that when they sleep in the recommended position, mornings feel easier. When positioning changes too early, the abdomen often feels tight and sore the next day.
Good sleep positioning protects the repair and makes recovery more predictable.
Video: Abdominoplasty AKA Tummy Tuck
Understanding the Anatomy That Is Healing
Several layers of the abdomen are involved in abdominoplasty.
✓ Skin
The outer covering of the abdomen. During surgery, excess skin is removed and the remaining skin is tightened.
✓ Fat
Fat sits between the skin and the muscle layer. Some fat may be reduced during surgery to improve contour.
✓ Fascia
Fascia is a strong connective tissue layer that acts like an internal support belt for the abdomen.
During surgery, the fascia may be tightened to repair rectus diastasis.
✓ Rectus Muscles
These are the two “six-pack” muscles that run up and down the front of the abdomen.
Between them is a seam of connective tissue. When this seam stretches, the muscles separate. This is called rectus diastasis.
Repairing this separation improves abdominal support.
During early recovery the repair needs protection from stretching.
Size vs Position vs Contour
Three different factors affect how the abdomen heals after surgery.
- Size
This refers to how much tissue is present.
Swelling after surgery temporarily increases abdominal size.
- Position
Position refers to where the abdominal tissues sit.
Sleeping position affects how gravity pulls on the abdomen.
- Contour
Contour refers to the shape of the abdominal surface.
Proper positioning reduces uneven swelling and helps contour settle more smoothly.
Understanding these differences helps patients understand why sleeping position matters during the first weeks.
The Best Sleeping Position After Abdominoplasty
The safest position after surgery keeps the body slightly bent.
This position is often called the “beach-chair position.”
In this setup:
- the upper body is elevated
- the knees are slightly bent
- the abdomen rests in a gentle curve
This position reduces tension across the abdominal repair.
It also allows the incision to relax rather than being pulled tight.
Patients can achieve this position using:
- a wedge pillow
- several regular pillows
- a recliner
- a powered lift chair
The furniture itself is not important.
The body position is what matters.
Using Pillows Correctly
Pillows are helpful tools during early recovery.
A simple setup usually includes:
✓ Behind the shoulders
This raises the upper body without forcing the neck forward.
✓ Under the knees
This keeps the hips and knees bent and reduces tension on the lower abdomen.
✓ Optional lower-back support
Some patients feel back fatigue when sleeping upright. A small pillow behind the lower back can improve comfort.
The goal is a stable shape that the body can relax into for several hours.
Using a Recliner or Lift Chair
Many patients find a recliner helpful during the first weeks.
A powered lift chair can make recovery easier because it:
- keeps the body in the recommended position
- helps patients stand without using their core muscles
- reduces twisting and straining
- makes nighttime bathroom trips easier
A lift chair is not required. It is simply a useful option for patients who want easier transitions from sitting to standing.
Getting In and Out of Bed Safely
Patients should avoid sitting straight up from a flat position.
This movement strains the abdominal repair.
The safest method is called the log roll.
To get out of bed
- Roll onto your side while keeping shoulders and hips moving together
- Let your legs slide off the bed
- Push up with your arms
To lie back down
Reverse the steps.
Practicing this movement before surgery makes it easier afterward.
Drains and Compression at Night
After surgery, drains help remove fluid from the surgical area.
During this phase the priority is proper drainage.
At Baumholtz Plastic Surgery:
- drains are typically used after abdominoplasty
- compression garments usually begin after drains are removed
While drains are present:
- keep tubing secured
- keep drain bulbs within reach
- avoid pulling or twisting the tubing while sleeping
Once drains are removed and swelling patterns are stable, compression garments may be introduced to improve comfort and support.
What the First Two Weeks of Sleep Are Like
Sleep often improves gradually over the first two weeks.
Nights 1–3
Expect:
- fragmented sleep
- frequent position adjustments
- mild tightness when moving
Walking during the day often improves sleep at night.
Nights 4–7
Most patients become more comfortable with the beach-chair position.
Small adjustments in pillow placement may improve comfort.
Week 2
Some patients can slightly reduce elevation if the abdomen feels relaxed.
If flattening causes tightness, return to the previous position.
Side Sleeping
Side sleeping is usually introduced after clearance from the office.
When allowed:
- keep the upper body slightly elevated
- place a pillow between the knees
- use a pillow along the abdomen to prevent twisting
Start with short trials. If soreness increases the next day, return to back-elevated sleep.
Flattening the Bed
Lowering the head of the bed should happen gradually.
Judge each change by:
- comfort during the night
- how the abdomen feels in the morning
- swelling patterns during the day
If tightness increases, return to the previous setup.
Sleep Environment Tips
Small environmental changes improve sleep quality.
Helpful steps include:
- keeping the room cool
- using breathable sheets
- using dim lighting for nighttime bathroom trips
- limiting bright screens before bed
- hydrating earlier in the evening
These steps reduce night disruptions and make positioning easier to maintain.
Lifestyle Factors That Affect Sleep and Healing
Certain habits slow healing and disrupt sleep.
These include:
- Nicotine
Nicotine reduces blood flow and delays wound healing.
- Alcohol
Alcohol fragments sleep and interacts with pain medications.
- Late caffeine
Caffeine late in the day can disrupt sleep cycles.
Consistency helps the body recover more efficiently.
Milestones in Returning to Normal Sleep
Recovery timelines vary, but many patients notice patterns.
Around 6 weeks
Sleeping with less elevation often becomes comfortable.
Side sleeping becomes easier.
Around 12 weeks
Many patients return to their normal sleep position.
The abdomen feels stronger and the repair more stable.
Frequently Asked Questions
Can I sleep in a recliner after surgery?
Yes. Many patients use a recliner during early recovery because it keeps the body in the recommended position.
Why can't I lie flat right away?
Lying flat stretches the abdomen and increases tension on the muscle repair.
When can I sleep on my side?
Usually after clearance from the office, often several weeks after surgery.
What if I wake up flat during the night?
Simply bend your knees and return to the supported position.
Can I sleep on my stomach?
Stomach sleeping is usually the last position to return.
Will sleeping position affect swelling?
Yes. Proper positioning helps swelling settle more evenly.
Can I share a bed with my partner?
Yes, but many patients use a body pillow to prevent accidental bumps.
Should I wear my compression garment while sleeping?
Only after drains are removed and the garment is recommended by the office.
How long will I need pillows?
Most patients use elevated positioning for several weeks.
Why does the abdomen feel tighter in the morning?
This often reflects stretching during the night. Adjusting sleep position usually improves it.
Can I nap during the day?
Yes. Short naps can help recovery as long as the same protective position is used.
Does sleep quality affect healing?
Yes. Sleep supports tissue repair, hormone regulation, and pain control.
PubMed References
- van Uchelen JH, Werker PMN, Kon M. The long-term durability of plication of the rectus sheath in abdominoplasty. Plast Reconstr Surg.
- Nahas FX. An aesthetic classification of the abdomen based on the myoaponeurotic layer. Plast Reconstr Surg.
- Mota P, Pascoal AG. Diastasis recti abdominis during pregnancy and postpartum. Phys Ther.
- Spitznagle TM, Leong FC. Prevalence of diastasis recti abdominis. Int Urogynecol J.
- Sperstad JB et al. Diastasis recti prevalence after pregnancy. Br J Sports Med.
- Chouchani ET. Sleep and tissue recovery following surgery. Sleep Med Rev.
- Gottrup F. Oxygen, wound healing, and infection risk. Ann Surg.
Closing
Sleeping position after abdominoplasty protects the abdominal repair while the tissues heal.
Gentle flexion, controlled movements, and consistent positioning reduce tension on the incision and make recovery more predictable.
Small habits - like using pillows correctly, avoiding twisting, and maintaining a stable sleep setup - often make the difference between a difficult recovery and a steady one.
A consultation with Dr. Michael Baumholtz in San Antonio can provide detailed guidance tailored to each patient’s surgery and recovery plan.