How To Reduce Risk, Choose The Right Plan, And Avoid The Mismatches That Cause Regret
For many women, the fear is not just surgery. It is the fear of getting it wrong.
They may want breasts that feel more balanced in clothes. They may want volume back after pregnancy or weight loss. They may want less heaviness, less pulling, or relief from bra strap grooves. They may want to feel comfortable in a swimsuit again without constantly adjusting padding or support.
And then the worry shows up:
That fear is understandable. Online stories are dramatic. Before-and-after photos are curated. Revision cases are emotional. And breast surgery affects how a woman feels every day in clothing, in intimacy, in movement, and in her own skin.
But here is the first important truth:
A poor outcome does not always mean a surgeon was careless, reckless, or technically incompetent.
And in real life, when women come into Dr. Michael Baumholtz’s office saying they were “botched,” the most common issue is not a dramatic technical disaster.
It is usually this:
The patient wanted X.
The surgeon could only realistically deliver Y.
Those two things never truly aligned.
That kind of mismatch is one of the most common causes of regret in breast surgery.
A woman may want a lifted result without lift scars.
She may want very large implants in thin tissue without long-term stretching.
She may want dramatic cleavage in a chest anatomy that does not naturally allow it.
She may want softness, upper fullness, and no rippling in tissue that cannot safely support that exact combination.
If those expectations and limits are not made clear before surgery, the result may later be labeled “botched” even when the deeper problem was miscommunication, not malpractice.
That does not mean technical complications are not real. They are.
But the safest way to reduce regret is to build a plan around:
- anatomy
- tissue quality
- realistic mechanical limits
- shared goals that are actually aligned
Dr. Michael Baumholtz, Plastic Surgeon in San Antonio, Texas, approaches breast surgery with that framework in mind. The goal is not just to operate well. The goal is to make sure the operation matches the actual problem and the patient understands what can and cannot be delivered safely.
Video: How To Think About Cosmetic Breast Surgery
What Does “Botched Breast Surgery” Usually Mean?
“Botched” is not a medical diagnosis. It is a patient word.
Women usually use it when something:
- looks wrong
- feels wrong
- healed poorly
- does not match what they thought they were choosing
- changed in a way they did not expect over time
That can mean very different things from one patient to another.
Common Problems Patients Describe As “Botched”
Some women mean:
- “My breasts look unnatural”
- “The implants sit too high”
- “One side dropped lower”
- “I can see rippling”
- “The cleavage is wrong”
- “The scars are too visible”
- “My breasts feel hard”
- “They do not look anything like I thought they would”
These usually fall into several broad categories:
Position problems
- implants too high
- implants too low
- implants too far apart
- implants too close together
- implants drifting toward the armpits
Contour problems
- too round
- too fake-looking
- visible edges
- rippling
- double bubble or double contour
Healing problems
- wide scars
- dark scars
- raised scars
- wound separation
Capsule problems
- tightness
- distortion
- hardness
- pain from capsular contracture
Why The Word “Botched” Can Be Misleading
Some of these problems are preventable. Some are known complications. Some are expectation problems. Some are anatomy problems. Some are healing problems.
That is why a “botched” result does NOT automatically mean:
- negligence
- poor technical skill
- malpractice
Sometimes the real issue is that the procedure did not match the problem.
Sometimes the issue is that the plan exceeded what the tissues could safely support.
Sometimes the issue is that the patient expected a result their anatomy could never hold.
So the better question is not:
The better question is:
That means reducing the risk of:
- malposition
- rippling
- scar problems
- implant overload
- poor procedure selection
- expectation mismatch
Ready for Surgery? Take Dr Baumholtz Breast Surgery Quiz
Why Do Breast Surgery Outcomes Go Wrong?
There are usually three major drivers.
1. The Wrong Operation Is Chosen For The Real Problem
Breast concerns are usually about one or more of these:
- size
- position
- contour
- weight/heaviness
If those are confused, the wrong operation may be chosen.
Example:
A woman with clear droop wants a fuller, lifted look.
She is offered implants only.
The implants add volume, but they do not reliably raise the nipple.
Over time, the breast may look heavier, not more lifted.
That is not always a technical mistake.
It is often a planning mismatch.
2. The Tissues Are Asked To Carry More Than They Can Support
This is one of the biggest long-term causes of disappointing breast surgery.
If an implant is too large or too heavy for:
- the skin
- the fold
- the tissue thickness
- the chest dimensions
then the result may stretch, drift, or thin over time.
That can lead to:
- bottoming out
- rippling
- lateral drift
- loss of upper support
- revision surgery
3. Recovery Does Not Protect Healing
The pocket and soft tissues need time to stabilize.
Too much stress too early can increase:
- bleeding
- swelling
- scar widening
- implant pocket stretching
- asymmetry
That is why recovery is part of the operation, not an afterthought.
The Most Common Cause of “Botched” in Real Life: Miscommunication
This deserves its own section because it is so common.
When women present to Dr. Baumholtz saying they were “botched,” the most common story is not:
It is more often:
Or:
Or:
That happens when:
- the patient wants X
- the surgeon can only safely deliver Y
- neither side fully closes that gap before surgery
Examples:
- wanting a lift without lift scars
- wanting large implants in tissue that cannot support them
- wanting cleavage that chest anatomy does not allow
- wanting upper fullness without accepting increased roundness
- wanting “natural” and “dramatic” at the same time in a body that cannot safely support both
This is why consultation quality matters so much.
A good consultation does not just ask what the patient wants.
It asks:
- what is the real problem?
- what tools actually solve it?
- what are the tradeoffs?
- what can be delivered safely?
- what can not be delivered safely?
That is how you reduce regret.
Breast Reduction Before and After Photos
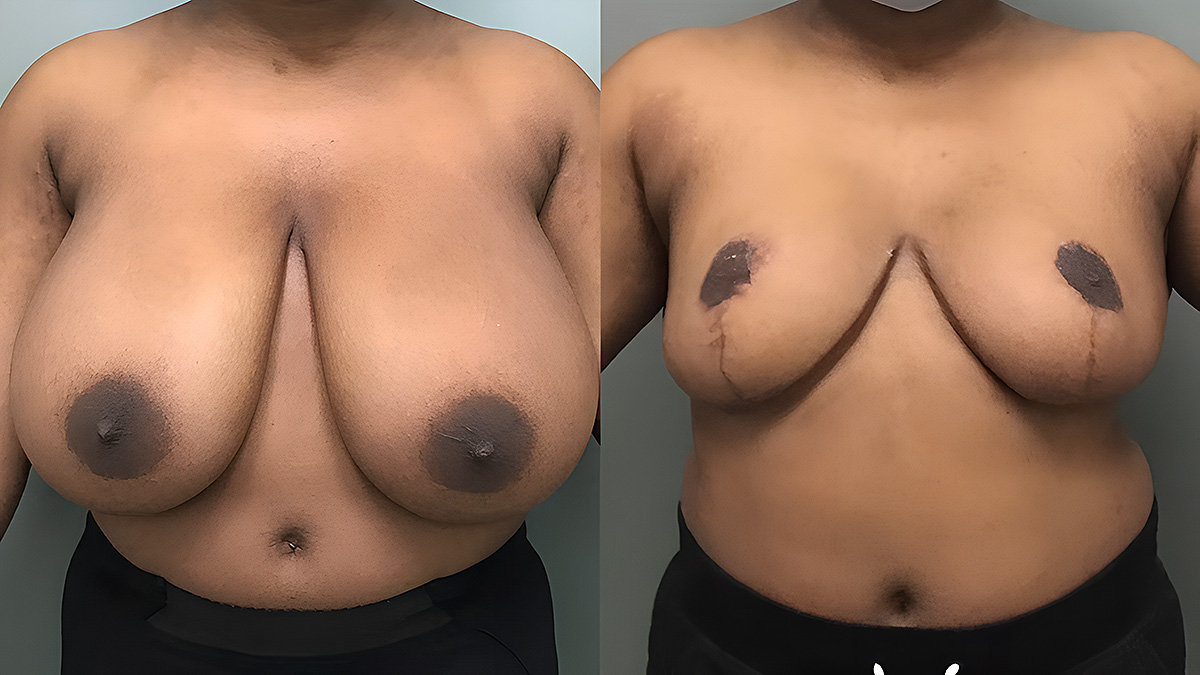
Visit Breast Reduction Gallery for More Before and After Photos
How Anatomy Should Guide the Plan
Breast surgery should be built around anatomy, not trends.
The Key Anatomy Terms Patients Should Understand
✓ Skin Envelope
The skin and soft tissue that act like a container for the breast.
If the skin is:
- thick
- supportive
- less stretched
it usually handles implants more predictably.
If it is:
- thin
- stretchy
- already over-expanded
it is less reliable as long-term support.
✓ Breast Base Width
This is the width of the breast footprint on the chest.
It matters because implants also have width.
A mismatch can cause:
- implants too wide
- implants too close to the center
- implants sitting too far apart
- unnatural side fullness
✓ Inframammary fold
This is the crease under the breast.
It is not just a line. It is a structural boundary. If it weakens, the implant can drift too low.
✓ Capsule
This is the scar layer the body forms around an implant.
That is normal.
Capsular contracture is when that scar tightens too much and distorts the implant or causes pain.
✓ Pectoralis major muscle
This is the chest muscle under the breast.
When surgeons say an implant goes “under the muscle,” they almost always mean dual-plane placement:
- part under the muscle
- part under the breast tissue
That is Dr. Baumholtz’s preferred technique for most augmentation patients because it often improves upper coverage and creates a smoother upper breast transition.
What Breast Surgery Can and Cannot Change
Breast surgery can:
- add volume
- reduce weight
- reposition the nipple with a lift
- remove extra skin
- improve contour
- rebuild weakened support in selected revision cases
Breast surgery cannot:
- change your ribcage
- create cleavage your chest anatomy does not allow
- guarantee perfect symmetry
- stop the aging process
- make tissue stronger than biology allows
Those limits are not bad news. They are what make a plan honest.
How to Choose the Right Procedure
✓ Breast Augmentation
Best when the real problem is volume loss and nipple position is still reasonable.
Breast Augmentation adds fullness. It does not reliably correct meaningful droop.
✓ Breast Lift (mastopexy)
Best when the real problem is position.
If the nipple sits low or points downward, a breast lift is usually the correct tool.
Trying to avoid lift scars by skipping the lift is one of the most common setups for disappointment.
✓ Breast Reduction
Best when the real problem is heaviness.
Breast reduction removes weight, improves shape, and often improves comfort in ways that patients feel every single day.
✓ Revision Surgery
Best when a prior surgery created a structural problem:
- bottoming out
- rippling
- malposition
- capsular contracture
- poor fold control
- rupture
- size mismatch that no longer fits the patient’s life
Breast revision surgery is usually more complex because tissues are scarred and support may be weaker.
Implant Selection: How to Avoid Long-Term Problems
✓ Why Cup Size Talk Is Risky
Cup sizes are not reliable planning tools.
There is no universal standard. Different bras fit differently. Different women wear bras differently.
That is why Dr. Baumholtz does not build a surgical plan around cup size.
✓ Why CC Talk Is Also Misleading
Implant “cc’s” are just the end result of width + projection + height relationships.
They are not the goal.
The real question is: What implant dimensions fit this chest safely and create the desired shape?
The Implant Variables That Matter
- width
- projection
- fill material
- tissue support
Width
Must match the breast base width.
Projection
Changes how far the breast projects forward.
Fill material
Saline and silicone feel different and behave differently in thin tissues.
✓ The “Too Big” Problem
This is one of the biggest causes of long-term disappointment.
Large implants can look appealing early. But over time, the weight matters.
Too much implant load can cause:
- tissue thinning
- stretching
- bottoming out
- rippling
- recurrent droop
- revision
That is why long-term planning matters more than the first few photos.
Rippling, Thin Tissue, and Structural Support
What Is Rippling?
Rippling is when implant folds become visible or palpable through thin tissue.
It is not dangerous, but it can be very disappointing.
How Rippling Can Be Reduced
- careful implant selection
- appropriate pocket choice
- respecting tissue limits
- using Alloclae in selected cases
Alloclae is donated structural fat available off the shelf. It can help improve soft tissue coverage in selected patients and may be useful in managing visible rippling.
When Internal Support Helps
Some patients benefit from internal mesh support (often called an internal bra) when:
- tissues are very thin
- implants are relatively heavy for the frame
- the fold is weak
- a lift needs more support
- revision surgery has damaged the internal support structures
This is not needed for every patient. It is used when the risk of tissue failure is already elevated.
Surgical Technique Matters
Technique affects:
- pocket control
- fold stability
- contamination risk
- bleeding control
- revision options later
Incision Choice
Many surgeons prefer the inframammary fold incision because it gives direct control over the pocket and can often be reused in revision.
Pocket choice
Pocket choice should match:
- tissue thickness
- goals
- implant characteristics
- long-term support needs
A pocket should not be chosen because it is trendy.
It should be chosen because it fits the anatomy.
Risk Reduction Steps
Modern breast surgery often includes:
- careful implant handling
- pocket irrigation
- antiseptic preparation
- controlled insertion methods
These steps reduce risk. They do not eliminate it.
What Patients Should Look For in a Surgeon
Patients should look for:
- board certification in plastic surgery
- real revision experience
- careful measurements during consultation
- willingness to say “no” when anatomy does not safely support the request
- clear explanation of tradeoffs
A safe consult should include:
- base width measurement
- tissue thickness assessment
- nipple position review
- skin quality discussion
- scar discussion
- realistic recovery explanation
Red Flags That Often Lead to Regret
Be cautious if a consultation includes:
- promises of a specific cup size
- dismissal of obvious droop without discussing lift
- implant suggestions that ignore tissue quality
- minimizing scar tradeoffs
- minimizing recovery restrictions
- oversized implant plans presented as if they have no long-term cost
How Patients Can Reduce Their Own Risk
Patients are not passive in this process.
Nicotine
Nicotine is one of the biggest controllable risks.
It reduces blood flow and increases:
- wound issues
- infection risk
- scar problems
- tissue breakdown
That includes:
- smoking
- vaping
- nicotine gum
- nicotine patches
- nicotine pouches
Weight Stability
Weight changes affect breast tissue and skin.
Chronic Health Conditions
Diabetes and other healing-related issues need to be optimized first.
Lifestyle Honesty
If a patient is highly active, hates bras, or wants to avoid future revision, that should influence the plan.
Recovery Mistakes That Can Lead to a “Botched-Looking” Result
The first few weeks matter.
Common mistakes:
- lifting too early
- starting workouts too soon
- ignoring garment instructions
- side sleeping too early in selected cases
- not calling when something suddenly changes
Early swelling can make implants look high or uneven. That can be normal.
But a sudden change in shape, redness, pain, or swelling deserves a call.
What to Do If You Think Your Result Is Botched
First, define the problem specifically.
Is it:
- position?
- contour?
- scar?
- firmness?
- size mismatch?
- nipple position?
- rippling?
That matters because the fix depends on the category.
Second, understand timing.
Some issues need early action:
- bleeding
- infection
- rapid one-sided swelling
Other issues should be evaluated after swelling settles.
Third, get a structured second opinion if needed.
A good second opinion includes:
- measurements
- implant review
- pocket evaluation
- fold stability assessment
- tissue thickness review
- honest discussion of what can be improved and what cannot be erased
FAQs About Avoiding Botched Breast Surgery
How can I tell if a consultation is truly customized?
A customized consultation includes measurements, tissue assessment, nipple position review, and a clear explanation of whether the problem is volume, position, contour, or heaviness. If the conversation only focuses on "how big," it is probably not customized enough.
Is a bad breast surgery result always malpractice?
No. A poor outcome is not automatically malpractice. Many disappointing results are caused by expectation mismatch, anatomy mismatch, healing problems, or known complications—not reckless or negligent surgery.
What is the most common cause of someone saying they were botched?
Miscommunication. In real life, the most common issue is that the patient wanted X, the surgeon could only safely deliver Y, and that mismatch was never clearly resolved before surgery.
What question should I ask to check if an implant plan is safe long term?
Ask whether the implant width matches your breast base width and how the plan protects the fold over time. That question reveals whether the plan is based on anatomy or just appearance goals.
Why do some results look okay in a bra but disappointing in a tank top?
A bra hides many problems by adding support and compression. Without it, issues like rippling, lateral drift, bottoming out, or poor spacing may become more obvious.
What causes implants to sit too far apart?
This can happen when implant width is too narrow for the desired effect, the pocket is dissected too laterally, or the patient's chest anatomy naturally has wider spacing than expected.
Why do implants sometimes look too close together?
An implant that is too wide for the chest or a pocket created too close to the center can crowd the midline and reduce natural separation.
What is bottoming out?
Bottoming out means the implant settles too low because the fold support weakens or the implant load exceeds what the tissues can hold.
What is a double bubble?
A double bubble is a double contour under the breast. It often happens when the implant and the natural breast tissue settle at different levels.
Why is rippling more common in some patients?
Rippling is more common in thin tissue because there is less soft tissue covering the implant. Implant type, size, and pocket choice also matter.
Can rippling be fixed?
Often it can be improved. Options may include implant exchange, pocket adjustment, tissue support changes, or using Alloclae in selected cases.
What is capsular contracture?
Capsular contracture is when the normal scar tissue around an implant tightens too much and causes firmness, discomfort, or shape distortion.
Is BIA-ALCL common?
No. It is rare. It has been associated mainly with certain textured implants, and many surgeons now prefer smooth implants to reduce that risk.
What symptoms should make me worry about BIA-ALCL?
The most common symptom is delayed swelling around the implant years after surgery, often from fluid buildup. A new lump can also be a sign that needs evaluation.
Why don't you use bra cup size in planning?
Because cup size is inconsistent and not standardized. It is not a reliable surgical measurement.
Why don't you focus on implant cc's?
Because cc's are only the end result of a formula involving width, projection, and height. The real goal is a safe shape on your body, not a number.
What if I want a very large implant?
That depends on your tissues. Large implants can be done in some patients, but if they exceed what the skin and support structures can safely hold, the long-term risk rises significantly.
Why would I need a lift if I'm getting implants?
Because implants add volume, but they do not reliably correct nipple position. If the nipple sits low, a lift is often the correct tool.
Can I avoid lift scars and still get a lifted look?
Sometimes a small amount of upper fullness can create the illusion of lift, but true droop usually requires a real lift. Avoiding the necessary lift is one of the most common paths to disappointment.
What is "under the muscle" really?
Most of the time it means dual-plane placement, where the implant is partly under the muscle and partly under the breast tissue—not fully buried under muscle.
Why is dual-plane placement often preferred?
Because it often gives better upper coverage, especially in thinner patients, while still allowing the implant to settle naturally in the lower breast.
When does internal mesh support help?
It can help when tissues are thin, implants are relatively heavy, the fold is weak, or a lift/revision needs extra support.
Can a botched-looking result happen even if surgery was technically well done?
Yes. If the plan did not match the real problem, or if expectations and anatomy were never aligned, the result may still feel wrong to the patient.
What recovery mistake most often causes trouble?
Doing too much too soon. Early overactivity can increase swelling, bleeding, scar widening, and pocket stretching.
What signs should make me call the office right away?
Sudden one-sided swelling, increasing redness, drainage, fever, worsening pain, or a rapid shape change.
How soon should a "botched" result be revised?
It depends. Some problems need early action. Others should wait until swelling settles and tissues soften. Timing is part of good revision planning.
What should I bring to a second opinion?
Any implant card, prior operative reports if available, and a timeline of what changed and when. Photos over time are helpful too.
Can revision fix everything?
Revision can often improve a lot, but it cannot always erase every sign of prior surgery. A good revision plan is honest about that.
How can I reduce my odds of needing revision later?
Choose a plan that respects anatomy, avoid oversizing, follow recovery instructions carefully, and work with a surgeon who is honest about tradeoffs.
What is the safest overall strategy to avoid a botched outcome?
Choose the right operation for the real problem, align goals honestly before surgery, and build the plan around what your tissues can safely hold over time.
Medical References
- Adams, W. P., Jr. (2017). Breast augmentation. Plastic and Reconstructive Surgery, 140(5S Advances in Breast Reconstruction), 7S–19S. https://doi.org/10.1097/PRS.0000000000003948
- Brody, G. S., Deapen, D., Taylor, C. R., Pinter-Brown, L., House-Lightner, S. R., Andersen, J. S., Carlson, G., Le, M., & Epstein, A. L. (2015). Anaplastic large cell lymphoma occurring in women with breast implants: Analysis of 173 cases. Plastic and Reconstructive Surgery, 135(3), 695–705. https://doi.org/10.1097/PRS.0000000000001032
- Clemens, M. W., & Horwitz, S. M. (2017). NCCN consensus guidelines for the diagnosis and management of breast implant-associated anaplastic large cell lymphoma. Aesthetic Surgery Journal, 37(3), 285–289. https://doi.org/10.1093/asj/sjw259
- Hammond, D. C. (2017). Discussion: The importance of pocket control in breast augmentation and revision breast augmentation. Plastic and Reconstructive Surgery, 140(4), 703e–704e. https://doi.org/10.1097/PRS.0000000000003705
- Lista, F., & Ahmad, J. (2013). Vertical scar mastopexy with breast augmentation: A practical approach. Aesthetic Surgery Journal, 33(2), 299–308. https://doi.org/10.1177/1090820X12474619
- Maxwell, G. P., & Gabriel, A. (2017). Breast implant design. Gland Surgery, 6(2), 148–153. https://doi.org/10.21037/gs.2016.11.09
- Spear, S. L., Dayan, J. H., Clemens, M. W., & Nahabedian, M. Y. (2014). The correction of capsular contracture by conversion to "neosubpectoral" pocket placement. Plastic and Reconstructive Surgery, 133(1), 13–20. https://doi.org/10.1097/01.prs.0000436515.47175.27
- Tebbetts, J. B. (2006). Dual plane breast augmentation: Optimizing implant-soft-tissue relationships in a wide range of breast types. Plastic and Reconstructive Surgery, 118(7 Suppl), 81S–98S. https://doi.org/10.1097/01.prs.0000237008.50974.81
- U.S. Food and Drug Administration. (2024). Risks and complications of breast implants. U.S. Department of Health and Human Services. https://www.fda.gov/medical-devices/breast-implants/risks-and-complications-breast-implants
- Wixtrom, R. N., Canady, J. W., Glicksman, C. A., & Maxwell, G. P. (2012). Managing complications in breast augmentation. Clinics in Plastic Surgery, 39(2), 157–171. https://doi.org/10.1016/j.cps.2012.01.005
Reasons to Choose Dr. Baumholtz for Breast Surgery
- Dual board-certified: Board Certified in Plastic Surgery and Board Certified in General Surgery
- Extensive complex reconstructive background: helpful in both primary surgery and revision surgery
- Experience with primary and revision aesthetic breast surgery
- Conservative, anatomy-first philosophy
- Straightforward communication about tradeoffs, not hype
- Accessibility through the office, by phone, and through the Symplast app
- Focus on long-term tissue behavior, not just early photos
Schedule a Consultation in San Antonio, TX
Women considering breast surgery in San Antonio should leave consultation with clarity - not sales pressure.
A consultation with Dr. Michael Baumholtz can help define:
- the real problem
- the right operation
- the realistic tradeoffs
- the safest long-term plan
That may mean augmentation.
It may mean a lift.
It may mean reduction.
It may mean revision.
The goal is not just change. The goal is a result that makes sense for your anatomy, your life, and your long-term comfort.
Furtheer Reading
- Read Dr Baumholtz's Blog on How is Breast Reduction Done? [Quick Guide]
- Read Dr Baumholtz's Blog on What is the Minimum Size for Breast Reduction [All You Need to Know]
- Read Dr Baumholtz's Blog on Understanding and Reducing Breast Augmentation Scars
- Read Dr Baumholtz's Blog on How to Reduce Swelling And Bruising After Breast Reduction Surgery